Osteoporotic Vertebral Fracture in Elderly in Singapore
Understanding serious causes of back pain in older adults and how timely treatment can protect independence and mobility
By Dr Lau LL | drlauspineclinic@gmail.com | Singapore | Published on 01 March 2026 | Last modified on 15 March 2026
The Scoliosis & Spine Clinic (SG) provides clinical evaluation and management for osteoporotic spine fractures — a common but often overlooked cause of sudden severe back pain in older adults. This page explains how these fractures occur, how to recognise red flags, and what treatment options are available in Singapore.
Back pain is very common in older adults. Many episodes are due to muscle strain or wear‑and‑tear changes in the spine. However, in the elderly—especially those with osteoporosis—sudden severe back pain after a minor fall may signal an osteoporotic spine fracture, a condition that can threaten mobility, confidence, and cherished travel plans.
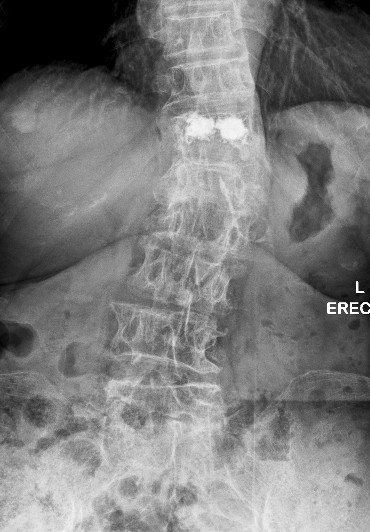
Common causes of back pain in the elderly
In older adults, back pain can arise from several overlapping conditions. Some are mild and self‑limiting, while others require urgent attention. Common causes include:
- Muscle strain and ligament sprain – often after overexertion, lifting, or unfamiliar activity.
- Degenerative disc disease – age‑related disc wear causing stiffness and mechanical back pain.
- Facet joint arthritis – “wear‑and‑tear” of the small joints at the back of the spine.
- Spinal stenosis – narrowing of the spinal canal causing back and leg pain when walking.
- Degenerative scoliosis – age‑related curvature of the spine causing imbalance, stiffness, and pain.
- Osteoporotic vertebral fracture – collapse of a weakened vertebra, often after a minor fall.
- Less common but serious causes – infection, tumour, or inflammatory conditions.
Among these, osteoporotic vertebral fractures are frequently under‑recognised. Patients may assume it is “just a sprain” and delay seeking care, despite severe pain and difficulty moving.
When back pain may be an osteoporotic spine fracture
Red flags in elderly back pain
- Sudden onset severe pain after a minor fall, slip, or even simple bending.
- Sharp, localised pain in the mid or lower back, worse when standing or walking.
- Difficulty turning in bed or getting in and out of a chair due to pain.
- Visible stooping or loss of height over time.
- Known osteoporosis or previous fragility fractures (wrist, hip, spine).
If these features are present, an osteoporotic vertebral fracture should be considered and early medical assessment is important.
What is vertebroplasty?
Vertebroplasty is a minimally invasive procedure used to stabilise painful osteoporotic spine fractures. Under imaging guidance, medical‑grade bone cement is injected into the fractured vertebra. This can:
- Stabilise the fracture and reduce painful micromovements.
- Provide rapid pain relief in appropriately selected patients.
- Improve mobility and allow earlier return to daily activities.
Vertebroplasty is not suitable for every fracture. Careful assessment with X‑rays and MRI/CT is needed to confirm the diagnosis, timing, and safety of the procedure.
Case story: From cancelled holiday to Antarctica
To illustrate how an osteoporotic spine fracture can affect life plans—and how treatment can restore independence—consider the story of an 80‑year‑old lady in Singapore.
Her fall, diagnosis, and pain
She was an active 80‑year‑old grandmother who loved travelling with her family. Like every morning, she headed to the nearby park for her routine exercises.
While avoiding a crowd, she tripped and fell hard on her buttock. She felt immediate, severe back pain and could not get up. Her helper and a passer‑by assisted her, and she was rushed to urgent care.
X‑rays and MRI revealed a T12 burst fracture, a serious osteoporotic injury, despite what seemed like a minor fall.
Vertebroplasty and pain relief
Her pain eased slightly when lying still, but every movement triggered sharp pain. A family holiday to Hong Kong the following week suddenly seemed impossible.
After discussing options, she chose vertebroplasty. Bone cement was injected into the fractured vertebra under imaging guidance. Risks—mainly cement leakage—were minimised through precise technique.
Her pain improved dramatically. She could sit, stand, and walk with far greater comfort. Although the Hong Kong trip was cancelled, she regained confidence and began osteoporosis treatment.
Back to living: Antarctica with her family
Two months later, she was strong enough to embark on a long‑awaited family trip to Antarctica—a once‑in‑a‑lifetime adventure she refused to miss.
One holiday was sacrificed, but timely diagnosis and vertebroplasty allowed her to return to meaningful activities and create unforgettable memories.

Two months after vertebroplasty, she traded hospital beds for icebergs—celebrating life with her family in Antarctica.
Key takeaways for elderly patients and families
- Do not ignore sudden severe back pain after a fall, even if the fall seems minor.
- Seek early assessment to rule out osteoporotic spine fractures and other serious causes.
- Timely treatment, including vertebroplasty in selected cases, can reduce pain and protect independence.
- Osteoporosis management—medications, nutrition, exercise, fall prevention—is essential to prevent future fractures.
Conclusion
Back pain in the elderly should never be dismissed as “just old age”—especially when it is sudden, severe, or follows a fall. Osteoporotic spine fractures are common but treatable. With careful evaluation and appropriate interventions, many patients can regain comfort, mobility, and the ability to participate in important family events and travel.
At The Scoliosis & Spine Clinic (SG), we provide comprehensive assessment for elderly back pain, including evaluation for osteoporotic fractures and discussion of both conservative and minimally invasive options such as vertebroplasty.
