Slipped Disc and Sciatica in Singapore
Understanding Symptoms, Red Flags, Causes and Treatment Options

Joe’s Story: When Back Pain Becomes Something More
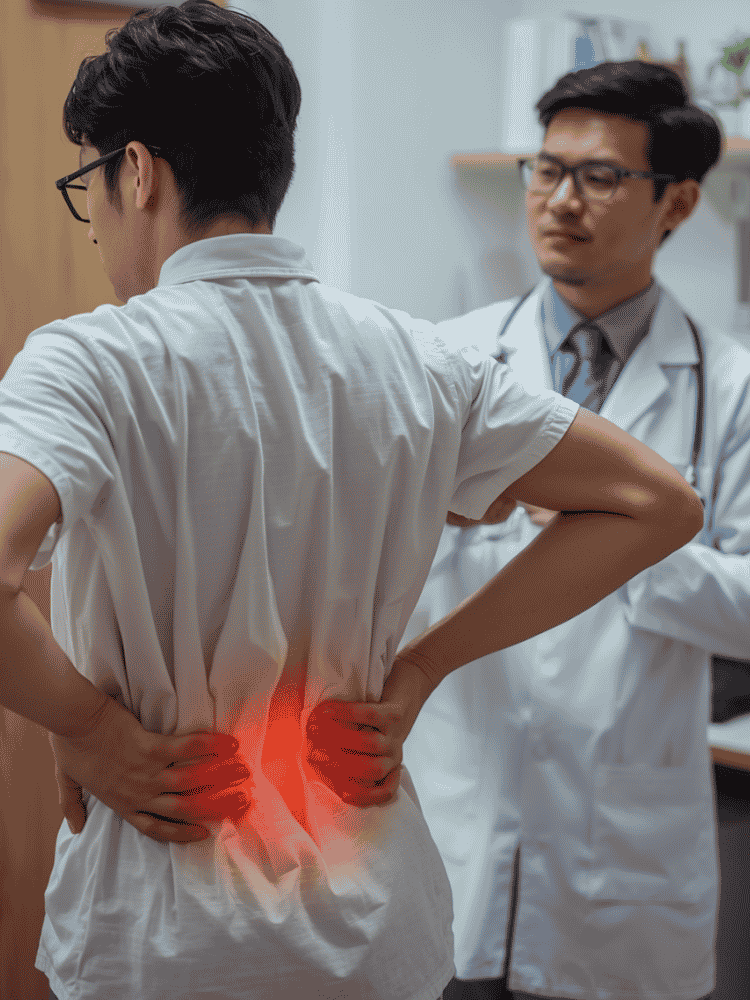
Many patients first experience back pain during periods of heavy activity, and they often assume it is just a muscle strain. Joe, a 35‑year‑old who had recently moved house, felt exactly that. After several days of lifting boxes and furniture, he noticed a persistent ache in his lower back. Over‑the‑counter painkillers helped a little, and he expected the discomfort to fade once the move was over.
A few days later, as he bent forward quickly to pick up a piece of clothing, a sudden, severe pain shot from his lower back into his right buttock and down his leg. The pain was so intense that he had to lie down immediately. Instead of easing, the radiating pain worsened, and his family called an ambulance. At the hospital, he was diagnosed with a prolapsed intervertebral disc—commonly known as a slipped disc—compressing the spinal nerves and causing sciatica.
Stories like Joe’s are common in Singapore. A slipped disc can occur after a single sudden movement or after weeks of accumulated strain. When the disc presses on the nerve roots, patients may experience back pain, buttock pain, leg pain, numbness, or weakness. Understanding how these symptoms develop and when to seek medical attention is essential for early recovery and long‑term spinal health.
In my clinical practice at Orthopaedic and Hand Surgery Partners, Gleneagles Hospital, I frequently see patients with slipped disc and sciatica—conditions that arise when a lumbar disc herniation compresses the spinal nerves. Patients often describe radiating leg pain, numbness, or difficulty walking. This article explains how these conditions present, what causes them, and how they can be treated effectively in Singapore.
What Are the Symptoms?
Joe’s experience reflects the typical progression of symptoms. What begins as a dull backache can evolve into sharp, shooting pain when the disc presses on the nerve roots. Patients often describe the pain as “electric,” “burning,” or “pulling,” especially when standing, coughing, or bending forward.
- Lower back pain or stiffness
- Radiating pain down the leg (sciatica)
- Numbness or tingling in the foot or calf
- Muscle weakness or foot drop
- Difficulty standing, walking, or climbing stairs
In more severe cases, patients may struggle to bear weight on the affected leg—just as Joe did when he could no longer stand without intense pain.
What Are the Risk Factors?
Joe’s situation highlights several common risk factors. Repetitive lifting, bending, and twisting place significant stress on the lumbar discs. When combined with fatigue, poor posture, or underlying disc degeneration, even a small movement can trigger a larger herniation.
- Age 30–60 (disc degeneration)
- Repetitive bending, lifting, or twisting
- Prolonged sitting or poor posture
- Smoking and reduced disc hydration
- Obesity and core muscle weakness
- Previous spine injury or surgery
Many patients are surprised that the “final trigger” is often something trivial—like picking up a sock—because the disc was already weakened from earlier strain.
What Causes Slipped Disc and Sciatica?
In Joe’s case, days of heavy lifting likely caused micro‑tears in the outer disc ring. When he bent forward suddenly, the weakened disc ruptured, allowing the inner gel to protrude and compress the nerve root. This is the most common mechanism behind acute sciatica.
- Herniated lumbar disc pressing on nerve roots
- Trauma or lifting injury
- Spinal instability or spondylolisthesis
Once the nerve is irritated, inflammation and swelling worsen the pain, which explains why symptoms often escalate rapidly within hours.
How Is It Diagnosed?
Some patients, like Joe, are diagnosed in the emergency department, but many are evaluated in a clinic setting. A careful clinical examination helps identify nerve tension, muscle weakness, and sensory changes. Imaging is used to confirm the diagnosis and guide treatment.
- Clinical examination (e.g. straight leg raise test)
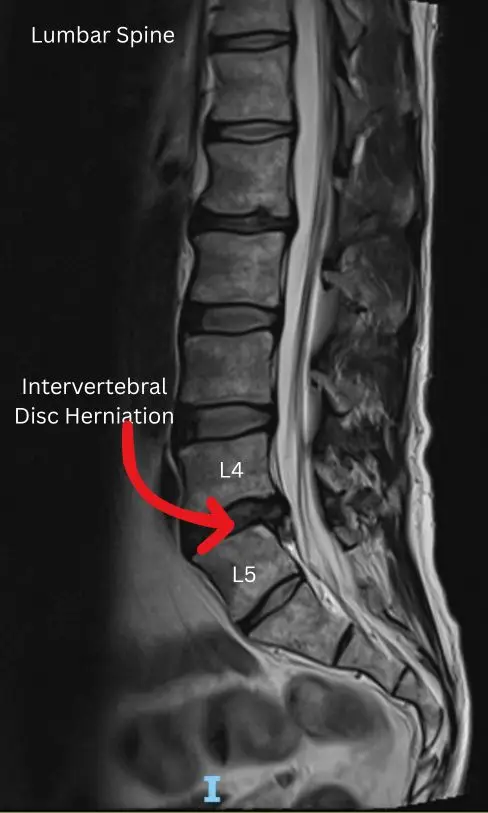
- MRI of the lumbar spine to confirm disc herniation
- CT scan for bony narrowing or foraminal stenosis
MRI remains the gold standard because it shows both the disc and the affected nerve root clearly.
Other Conditions That Can Mimic Sciatica
Not all buttock or leg pain comes from a slipped disc. Several non‑spinal conditions can produce similar symptoms and should be considered during assessment.
- ITB Tightness – Causes outer thigh or knee pain, often in runners. Usually no numbness or true nerve symptoms.
- Piriformis Syndrome – Tightness of the deep gluteal muscle compresses the sciatic nerve, causing buttock pain worsened by sitting.
- Sacroiliac Joint (SIJ) Dysfunction – Produces buttock pain that may radiate down the leg, especially when standing from a seated position.
- Hip Conditions – Hip arthritis or labral tears can refer pain to the groin, thigh, or buttock, but rarely cause numbness or weakness.
- Hamstring Tendinopathy – Deep buttock pain in athletes, worse with running or prolonged sitting.
These conditions differ from true sciatica because they typically lack nerve‑related symptoms such as numbness, tingling, or weakness. A focused clinical examination helps distinguish between spinal and non‑spinal causes.
What Are the Treatment Options?
Most patients, including those with severe initial pain like Joe, improve with structured non‑surgical care. The goal is to reduce inflammation, relieve nerve pressure, and restore mobility safely.
Non‑Surgical Management
- Activity modification and ergonomic correction
- Physical therapy and core strengthening
- Oral medications (NSAIDs, nerve modulators)
- Epidural steroid injections for inflammation
Many patients recover within weeks to months with the right combination of rest, physiotherapy, and targeted medication.
Surgical Intervention
Surgery is considered when symptoms persist despite conservative treatment, or when there is significant weakness, severe nerve compression, or difficulty walking. Early imaging and assessment help determine whether urgent surgery is needed.
- Microdiscectomy (minimally invasive disc removal)
- Lumbar decompression and fusion (for instability)
- Endoscopic discectomy (select cases)
Modern minimally invasive techniques allow many patients to return to normal activities much faster, with excellent long‑term outcomes.
Conclusion
Slipped disc and sciatica can significantly affect mobility, comfort, and quality of life. Joe’s experience shows how quickly symptoms can escalate—and how important early assessment is. With timely diagnosis, appropriate imaging, and a tailored treatment plan, most patients can achieve good pain relief and return to their usual activities.
If you are experiencing persistent back or leg pain, numbness, or weakness, especially with red‑flag symptoms, it is important to seek professional evaluation rather than waiting for the pain to “settle on its own”.
Frequently Asked Questions: Sciatica
What is sciatica?
Sciatica refers to pain caused by irritation or compression of the sciatic nerve—the largest nerve in the body—which runs from the
lower back through the buttock and down the leg. When a lumbar disc herniates or when the spinal canal narrows, the nerve becomes
inflamed, leading to radiating leg pain, numbness, or weakness.
Can scoliosis cause sciatica?
Yes. Scoliosis can shift the spine’s alignment and alter weight distribution, increasing pressure on the nerve roots. In adults,
degenerative scoliosis or disc collapse on the concave side of the curve can lead to nerve compression and sciatica‑like symptoms.
What are the red flags associated with sciatica?
Red flags suggest a more serious underlying condition and require urgent medical attention:
- Sudden or severe weakness in the leg or foot
- Loss of bladder or bowel control (possible cauda equina syndrome)
- Progressive numbness or neurological deficits
- Unrelenting pain that does not improve with rest or medication
- History of cancer, unexplained weight loss, fever, or infection
If any of these symptoms occur, seek emergency care immediately.
What are the typical symptoms of sciatica?
Patients often describe sharp, burning, or electric pain radiating from the lower back into the buttock, thigh, or calf. Numbness,
tingling, or muscle weakness may accompany the pain. Symptoms often worsen with sitting, bending forward, coughing, or twisting.
What is Cauda Equina Syndrome?
Cauda Equina Syndrome is a rare but serious condition caused by severe compression of the nerve bundle at the base of the spine.
It can lead to permanent neurological damage if not treated promptly.
- Sudden loss of bladder or bowel control
- Severe or rapidly worsening leg weakness
- Numbness in the saddle region (inner thighs, buttocks, genitals)
- Sharp or shooting pain in both legs
- Sexual dysfunction or loss of sensation
If you experience these symptoms, seek emergency medical attention immediately. Early surgical decompression is critical to prevent permanent deficits.
Who should I see for sciatica?
Persistent or worsening sciatica should be evaluated by an orthopaedic surgeon with a special interest in spine conditions
or a spine surgeon (orthopaedic or neurosurgical). These specialists are trained to diagnose nerve compression,
interpret MRI findings, and recommend appropriate treatment.
- Expertise in spinal anatomy and nerve‑related pain
- Accurate interpretation of MRI and imaging studies
- Access to minimally invasive and advanced surgical options
- Collaboration with physiotherapists and pain specialists
- Experience managing slipped discs, stenosis, and scoliosis‑related nerve compression
What is the recovery period for successful non‑operative treatment?
Most patients improve within 6 to 12 weeks with conservative care. Physiotherapy focuses on core strengthening, flexibility,
posture correction, and nerve mobilisation. Medications and activity modification help reduce inflammation and allow the nerve to recover.
When is surgery recommended?
Surgery is considered when:
- Symptoms persist beyond 6–12 weeks despite conservative treatment
- There is significant or progressive weakness
- Imaging confirms a surgically correctable disc herniation or stenosis
The most common procedure is a microdiscectomy, which removes the herniated disc fragment pressing on the nerve.
What is the recovery time after surgery?
Recovery varies by patient and procedure. Most individuals return to light activities within 4–6 weeks and resume fuller activity
within 2–3 months. Minimally invasive techniques often result in less pain and faster recovery.
How much does sciatica surgery cost?
Costs vary depending on hospital class, complexity, and insurance coverage. In Singapore’s private sector, a lumbar discectomy
typically ranges from SGD 20,000 to SGD 40,000. Public sector costs may be lower with subsidies. Always consult
your provider for an accurate estimate based on your condition and insurance plan.
Can I return to sports after treatment?
Yes. With proper rehabilitation and medical clearance, many patients return to sports and physical activity. Targeted physiotherapy
helps rebuild strength, improve flexibility, and reduce the risk of recurrence.
Does the clinic assist with insurance claims?
At Orthopaedic and Hand Surgery Partners, the clinic team can assist with insurance documentation and claims where appropriate.
- Support with insurance form completion
- Provision of medical reports and itemised invoices
- Coordination with major insurance providers
- Guidance on pre‑authorisation requirements
- Assistance with Medisave and Integrated Shield Plans (where applicable)
This helps streamline the process so you can focus on recovery.
How do you approach sciatica care?
In my practice, I use a multidisciplinary approach that combines orthopaedic expertise, physiotherapy, ergonomic guidance, and
personalised treatment planning. Whether non‑operative or surgical, the goal is to relieve pain, restore function, and support
long‑term spine health.
