Back pain is very common in older adults. Many episodes are due to muscle strain or wear‑and‑tear changes in the spine. However, in the elderly—especially those with osteoporosis—sudden severe back pain after a minor fall may signal an osteoporotic spine fracture, a condition that can threaten mobility, confidence, and cherished travel plans.
Common causes of back pain in the elderly
In older adults, back pain can arise from several overlapping conditions. Some are mild and self‑limiting, while others require urgent attention. Common causes include:
- Muscle strain and ligament sprain
- Degenerative disc disease
- Facet joint arthritis
- Spinal stenosis
- Degenerative scoliosis
- Osteoporotic vertebral fracture
- Less common but serious causes
Among these, osteoporotic vertebral fractures are frequently under‑recognised. Patients may assume it is “just a sprain” and delay seeking care, despite severe pain and difficulty moving.
When back pain may be an osteoporotic spine fracture
Red flags in elderly back pain
- Sudden onset severe pain after a minor fall or simple bending.
- Sharp, localised pain in the mid or lower back.
- Difficulty turning in bed or rising from a chair.
- Visible stooping or loss of height.
- Known osteoporosis or previous fragility fractures.
If these features are present, an osteoporotic vertebral fracture should be considered and early medical assessment is important. For enquiries, you may reach Dr Lau via the contact page.
What is vertebroplasty?
Vertebroplasty is a minimally invasive procedure used to stabilise painful osteoporotic spine fractures. Under imaging guidance, medical‑grade bone cement is injected into the fractured vertebra. This can:
- Stabilise the fracture
- Provide rapid pain relief in selected patients
- Improve mobility and allow earlier return to daily activities
Vertebroplasty is not suitable for every fracture. Assessment with X‑rays and MRI/CT is needed to confirm the diagnosis and timing.
Case story: From cancelled holiday to Antarctica
To illustrate how an osteoporotic spine fracture can affect life plans—and how treatment can restore independence—consider the story of an 80‑year‑old lady in Singapore.
Her fall, diagnosis, and pain
She was an active 80‑year‑old grandmother who loved travelling with her family. One morning, she tripped and fell on her buttock while avoiding a crowd. She felt immediate, severe back pain and could not get up.
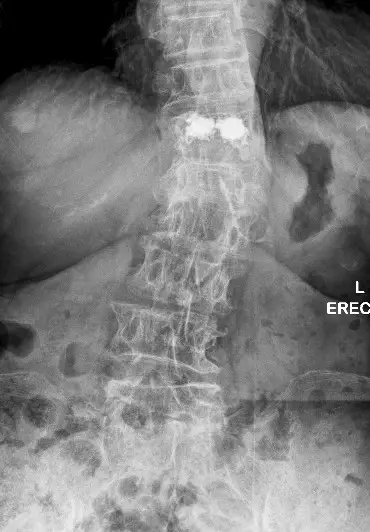
X‑rays and MRI revealed a T12 burst fracture, a serious osteoporotic injury.
Vertebroplasty and pain relief
Her pain eased slightly when lying still, but every movement triggered sharp pain. A family holiday to Hong Kong the following week seemed impossible.
After discussing options, she chose vertebroplasty. Bone cement was injected under imaging guidance.
Her pain improved dramatically. She regained confidence and began osteoporosis treatment.
Back to living: Antarctica with her family
Two months later, she was strong enough to embark on a long‑awaited family trip to Antarctica.

Two months after vertebroplasty, she traded hospital beds for icebergs—celebrating life with her family in Antarctica.
Key takeaways for elderly patients and families
- Do not ignore sudden severe back pain after a fall, even if the fall seems minor.
- Seek early assessment to rule out osteoporotic fractures and other serious causes of back pain.
- Timely diagnosis helps guide appropriate treatment options and supports mobility and independence.
- Osteoporosis management—including medication, nutrition, exercise, and fall‑prevention strategies—is important to reduce the risk of future fractures.
- Procedures such as vertebroplasty may help selected patients with persistent, severe pain, but they are not suitable for everyone. Decisions depend on the type of fracture, timing, imaging findings, and overall health.
For further questions, you may reach Dr Lau via the contact page.
Conclusion
Back pain in the elderly should never be dismissed as “just old age”—especially when it is sudden, severe, or follows a fall. Osteoporotic spine fractures are common but treatable. With careful evaluation and appropriate interventions, many patients can regain comfort, mobility, and the ability to participate in important family events and travel.
Learn more about spine conditions affecting older adults on the Geriatric Spine Conditions page.
FAQ
1. What causes an osteoporotic vertebral fracture?
These fractures occur when weakened bone can no longer tolerate normal daily forces. Simple actions such as bending forward or lifting light objects may trigger a collapse.
2. What symptoms suggest a vertebral fracture?
Sudden mid‑back or lower‑back pain is common. Some people notice difficulty standing upright or a new stooped posture. Persistent back pain in an older adult should be assessed by a healthcare professional.
3. Do all vertebral fractures require surgery?
Most do not. Many patients improve with rest, bracing, activity modification, and pain‑relief strategies. Surgery is considered only when pain remains severe or when the fracture causes nerve compression.
4. How long does recovery usually take?
Pain often improves over several weeks, but full recovery may take a few months depending on age, bone quality, and overall health.
5. Can another fracture be prevented?
Prevention focuses on treating underlying osteoporosis, improving balance and muscle strength, and reducing fall risks at home.
6. What surgical options are available?
Vertebroplasty, kyphoplasty, and stabilisation procedures may be considered depending on severity and symptoms.
7. Should elderly patients stay active after a fracture?
Gentle, guided movement is usually encouraged once acute pain settles. A clinician or physiotherapist can recommend safe exercises.
Disclaimer: This article provides general medical information and is not a substitute for professional assessment. For personalised advice, please consult a qualified healthcare professional.
