Explore Related Spine Guides
These articles form part of our comprehensive spine education series:

Spine care across all ages

Spine care across all ages
By
Dr Lau Leok Lim
| Orthopaedic & Spine Surgeon, Singapore
Published: 3 September 2025 | Last reviewed: 16 March 2026
Degenerative Disc Disease (DDD) is one of the most common causes of neck and lower back pain. This guide explains how discs age, how degeneration is graded on MRI, and what treatment options are available in Singapore.
These articles form part of our comprehensive spine education series:
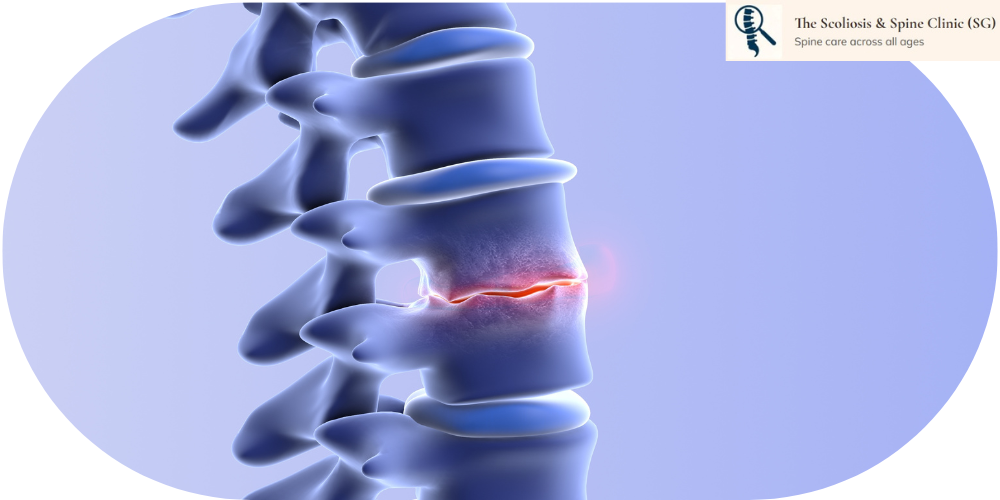
Degenerative Disc Disease – Age‑related disc dehydration and height loss
Degenerative Disc Disease (DDD) is a misnomer. It is not a disease, but a natural age‑related process where the intervertebral discs gradually lose hydration, height, and structural integrity. The spinal disc is often considered the weak link of the spinal column because it is the first structure to show signs of ageing.
Each disc functions as a shock absorber, allowing the spine to bend, twist, and carry load. Unlike most tissues in the body, the disc has no direct blood supply. Instead, it receives nutrients through diffusion across the vertebral endplates. As this diffusion becomes less efficient with age, the disc progressively dehydrates and degenerates.
Sometimes, patients experience a sudden worsening of symptoms — known as an exacerbation of DDD. This does not mean the disc suddenly “aged overnight.” Instead, it usually happens when a recent event places extra pressure on an already weakened disc. Examples include lifting something heavy, a sudden twist, prolonged sitting, or even a minor slip.
Disc degeneration follows a predictable pattern. Mild thoracolumbar disc degeneration can already be seen in individuals in their 20s. As people enter their 40s and beyond, the process accelerates, with more pronounced disc dehydration and disc height narrowing.
The L4/L5 level is most commonly affected due to its high mechanical load and mobility. The degree of disc height loss correlates strongly with the severity of disc degeneration.
| Grade | Description |
|---|---|
| Grade 1 | Mild disc dehydration, preserved disc height, no nerve compression |
| Grade 2 | Moderate disc height loss, annular fissures, early osteophytes |
| Grade 3 | Severe disc collapse, disc bulge or herniation, possible nerve root contact |
| Grade 4 | Advanced degeneration with Modic changes, spinal instability, or stenosis |
Degenerative Disc Disease – Educational Video
1. Is degenerative disc disease reversible?
No. Disc degeneration cannot be reversed, but symptoms can be effectively managed with targeted treatment.
2. Does disc degeneration always cause pain?
Not necessarily. Many people have disc degeneration on MRI without symptoms.
3. Can exercise help?
Yes. Core strengthening, flexibility training, and posture correction can reduce pain and improve function.
4. When should I see a spine specialist?
If pain persists beyond 6–8 weeks, radiates to the limbs, or affects daily activities, a specialist evaluation is recommended.
5. Does disc degeneration always lead to surgery?
No. Most patients improve with non‑surgical treatment. Surgery is reserved for severe nerve compression or instability.